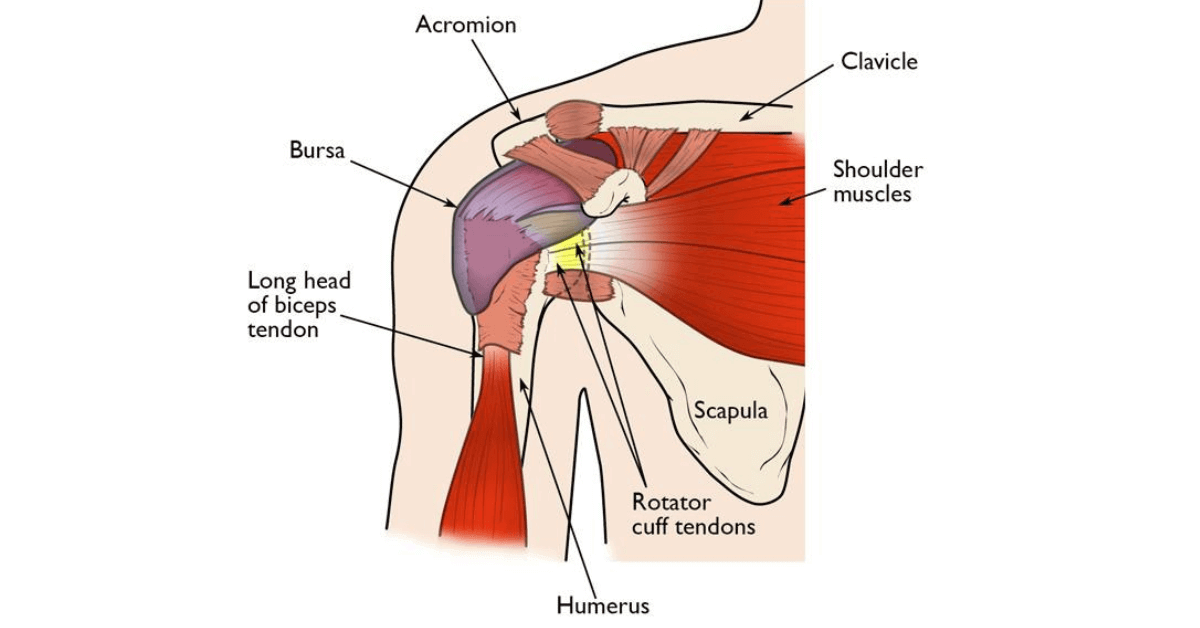
What Is a Rotator Cuff Tear?
The rotator cuff is a group of four tendons stabilising the shoulder. Tears can be partial or full-thickness, leading to pain, weakness, and difficulty lifting the arm. Arthroscopic repair reattaches the tendon to bone, restoring strength and preventing progression to cuff arthropathy.
Types of Cuff Repairs
- Single-row repair: For small tears with good tissue quality.
- Double-row or speed-bridge: Provides broad footprint coverage for medium to large tears.
- Partial repair & margin convergence: Optimises tension when full coverage is not possible.
- Tendon transfers or superior capsular reconstruction: Options for massive irreparable tears.
Who Needs Rotator Cuff Surgery?
Not all tears need surgery, but intervention is recommended when:
- Persistent pain: Night pain and weakness despite physiotherapy and injections.
- Acute traumatic tears: Sudden weakness after injury, especially in active adults.
- Large or retracted tears: Risk of progression to irreparability if left untreated.
- Occupational demands: Jobs requiring overhead labour or athletic pursuits.
MRI or high-resolution ultrasound evaluates tendon quality, retraction, and muscle atrophy to plan repair strategy.
Arthroscopic Repair Workflow
Minimally invasive techniques minimise pain and accelerate recovery.
- Portals & diagnostic scope: Evaluate bursa, biceps, labrum, and cartilage.
- Tendon preparation: Debridement and mobilisation of the torn cuff.
- Footprint preparation: Bone bed is freshened to stimulate healing.
- Suture anchor fixation: Sutures secure the tendon in single or double rows, often with biologic augmentation.
Benefits of Timely Repair
- Pain reduction: Eliminates night pain and improves sleep.
- Strength restoration: Reattached tendons regain power for lifting and sport.
- Joint preservation: Prevents progression to cuff arthropathy and shoulder replacement.
- Custom rehab: Programmes tailored to athletic or occupational goals.
Rehab Timeline
- Weeks 0–4: Sling support, passive range-of-motion, and scapular activation.
- Weeks 5–8: Assisted and active motion, gentle isometrics.
- Months 3–4: Progressive strengthening, closed-chain exercises, and proprioception drills.
- Months 5–6: Sport-specific or occupational conditioning.
- Month 6 onwards: Full return to heavy lifting, swimming, or racquet sports once cleared.
Risks & Management
Rotator cuff surgery is safe when performed by experienced arthroscopists.
- Re-tear: Minimized with proper technique, biological augmentation, and adherence to rehab timelines.
- Stiffness: Prevented through early motion protocols and pain control.
- Infection: Extremely rare; we follow strict sterile protocols and postoperative care.
- Nerve irritation: Protected through precise portal placement and intraoperative vigilance.
- Residual weakness: Addressed with long-term strengthening and scapular mechanics training.
Comprehensive follow-ups, ultrasound assessments, and rehab reviews keep your shoulder progressing safely.
